Fogarty Scholar: Coco and Joe from NPGH Fogarty Fellows on Vimeo.

Anya Romanoff spoke on the local news in Cusco, Peru to encourage women to get screened for breast cancer and engage in healthy lifestyles as part of her project.

Peter Donkor, MD MPH is a Professor of Oral and Maxillofacial Surgery at the Kwame Nkrumah University of science and Technology in Kumasi, Ghana and is also Pro Vice-Chancellor. He has earned degrees, fellowships, and diplomas from six different colleges, taught at the University of Sydney and the University of Birmingham, and served on numerous advisory boards throughout his productive career.
Ghana, an African country of 25 million inhabitants is located 80 north of the Equator and 20 west of the Prime Meridian. This uniquely places it closest to the center of the earth, with her citizens being among the friendliest in the world. Other unique features about Ghana include the hand woven kente cloth; the Volta Lake (a large man-made lake); “red-red”, a favorite local dish; open drains, and mini-buses inscribed with social, religious and political messages.
The buses which are mostly used are “home second-hand” imports from Europe, and form the backbone of the public transportation system that includes vehicles that have been written off in their countries of origin either after an accident or because they are unserviceable. These buses often also serve as ambulances for the transport of the seriously ill or injured to health facilities.
Mechanics in Ghana have developed skills for restoring “dead” vehicles regardless of their state. Thus rusty old vehicles get patched up and rendered “roadworthy”. A Mercedes Benz car with a failed engine may get refitted with a used but functional Toyota engine, while the rusty frame of a Mazda vehicle may be replaced with a newer Nissan one. In the same manner that imported used clothing keeps the not-so-well-off in Ghana decently attired, imported used vehicle tires keep vehicles moving on the very poor road network across the length and breadth of the country. Like many developing countries, injuries from road crashes contribute disproportionately to the burden of disease, and undoubtedly dilapidated vehicles contribute significantly to the problem.
Over the past twenty years one NIH/FIC funded research collaboration between the University of Washington (UW) in Seattle and the Kwame Nkrumah University of Science and Technology (KNUST) in Kumasi has focused on injury control. Activities under this collaboration have included driver education in first aid and safe transport of the injured; training of district medical officers in emergency surgical procedures; teaching of undergraduate medical students in trauma; workshops for media practitioners, police, fire personnel, lawyers, judges, parliamentarians, surgeons, social workers, engineers etc. Several Ghanaian graduates have gained MPH degrees in injury research, and faculty exchanges have also taken place.
Domestic violence, unintentional injuries such as accidental ingestion of chemicals by children, burns, suicide, and road traffic injuries require the combined efforts of law enforcement agencies, engineers, medical personnel, law makers, policy makers, researchers, and international agencies for effective control. Efforts at controlling this menace in Ghana require a multi-pronged approach and must include a strengthening of the entire health system. In an increasingly globalized world, international collaboration is a sine qua non. The recent Ebola epidemic in West Africa, and the threat it poses to the entire global community is a reminder that unless we collaborate internationally to solve global health problems, we stand the risk of perishing together. Therefore, as we celebrate the successes of the UW/KNUST collaboration, greater efforts are needed for extending the gains to benefit more communities.
This article was originally published in the NPGH Fogarty Fellows October 2014 Newsletter

Ronald Maio, DO, MS, FACEP founded and directed the University of Michigan Injury Research Center, and was PI for the Great Lakes Node of the Pediatric Emergency Care Applies Research Network. He is currently Professor Emeritus in Emergency Medicine at the University of Michigan Medical School.
On my recent trip to Ghana this past August, much of the country’s concern, and rightfully so, was focused on the Ebola crisis raging within its neighboring countries. However, the day before I returned to the US, the pernicious problem of death and disability from traumatic injuries, a problem that is my particular research interest and that of my mentees, came to the fore. There was a tragic road accident involving three mini-vans outside of Kumasi on the Kumasi to Accra Highway. Twenty-three people died and 11 others were injured. Twenty-one of those people were dead at the scene and two died in hospital. The dead and injured consisted primarily of young adults and children.
Death and disability from traumatic injuries, particularly road accident related injuries, have become a leading cause of death and disability in the developing world, and continue to be a major cause of death and disability within industrialized countries. The overwhelming majority of its victims are those that are in the early years of their productive adult life. As an emergency physician, a large portion of my training and practice focused on the evaluation and treatment of patients with traumatic injuries. My early research also focused on this area, but I eventually realized an important fact that the above described accident illustrates: most of the people that die from traumatic injuries, particularly road accidents, die immediately from catastrophic injuries. Most notably these are severe brain, cervical spinal cord and thoracic aorta injuries.
While I knew the importance of timely and high quality medical care for the injured patient, it became clear to me that I wasn’t doing enough. I needed to include prevention activities in my practice and in my research. My thinking was strongly influenced by the concepts of primary, secondary and tertiary prevention and the Haddon Matrix for injury control. This matrix can be applied to all injury events but was initially used for road accidents. It helps organize factors leading to an accident, and by filling the cells of the matrix one can develop both general and specific strategies for intervention.
At the time my perspective was broadening there were still many silos in the US addressing injuries from road accidents: it’s an engineering problem; it’s a policy problem; it’s a regulation problem; it’s a law enforcement problem; it’s a health behavior/ health education problem; and of course, it’s a medical problem. Thanks to the CDC’s National Center for Injury Prevention and Control and my early mentors and colleagues, I came to realize that death and disability from traumatic injuries is best addressed as a public health problem that requires co-ordinated multifaceted solutions. I began to collaborate with other Departments within the University of Michigan Medical School (UMMS) as well as the UM School of Public Health, the University of Michigan Transportation Research Institute, and the School of Pharmacy. 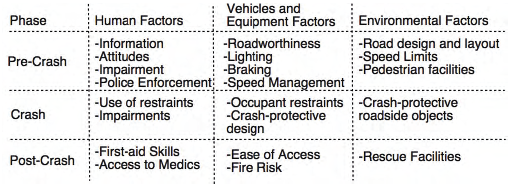
Although my research in acute trauma care continued, I also began conducting research on using computer technology to identify alcohol problems and intervene among the complete range of injured adults and adolescents presenting to the Emergency Department. An underlying concept was our perspective that a visit to the Emergency Department for an injury was a “teachable moment” to address risky behavior that could result in future injuries. Subsequently, my colleagues have expanded our work on alcohol problems to include addressing risk factors for inter-personal violence and seatbelt use. In the US, during the last 20 years, there has been a dismantling of the aforementioned “silos” and the growth of inter-disciplinary collaboration: essentially a team approach to the public health problem of traumatic injuries from road accidents.
As we help fellow global citizens in developing countries address the problem of traumatic injury in a sustainable fashion, we need to take a similar team approach. A great example of such an approach is the work that Dr. Charles Mock, a trauma surgeon from the University of Washington (UW), and his colleagues at the UW and in Ghana have been doing in the area of traumatic injury. Their work not only addresses acute clinical care issues, but also behavioral and environmental risk factors and is inter-disciplinary in nature.
We are fortunate to have the work of Dr. Mock and his colleagues on which to build and be informed, as well as his assistance with studies on quality of trauma care and also development of a trauma registry at Komfo Anokye Teaching Hospital (KATH), Kumasi, Ghana. These projects were headed and recently completed by Dr. Rocky Oteng, faculty in the UMMS Department of Emergency Medicine, during his Fogarty Research Fellowship. We are also conducting a project to determine the frequency of alcohol use and risky drinking among trauma patients presenting to KATH. This work is being conducted by a current Fogarty Fellow, Andrew Gardner, an M-3 at UMMS. We are also very fortunate to have the collaboration and co- leadership on these projects from the Director of Accident and Emergency (A and E) at KATH, Dr. George Oduro, and A and E faculty member Dr. Paa Kobina Forson. We think our work will have implications not only for acute clinical care but also for policy and prevention activities. We also think it will serve as a platform on which to further develop a sustainable research enterprise to reduce death and disability from traumatic injury in Ghana as well as the rest of Sub-Sahara Africa—and beyond!
My colleagues at the University of Michigan and our Ghanaian colleagues at KATH are very excited about our work and also very excited and proud to be part of the Global Team to reduce death and disability from traumatic injuries.
This article was originally published in the NPGH Fogarty Fellows October Newsletter
Powered by WordPress & Theme by Anders Norén